Knee Cartilage Injury (Osteochondral Defect)
Overview
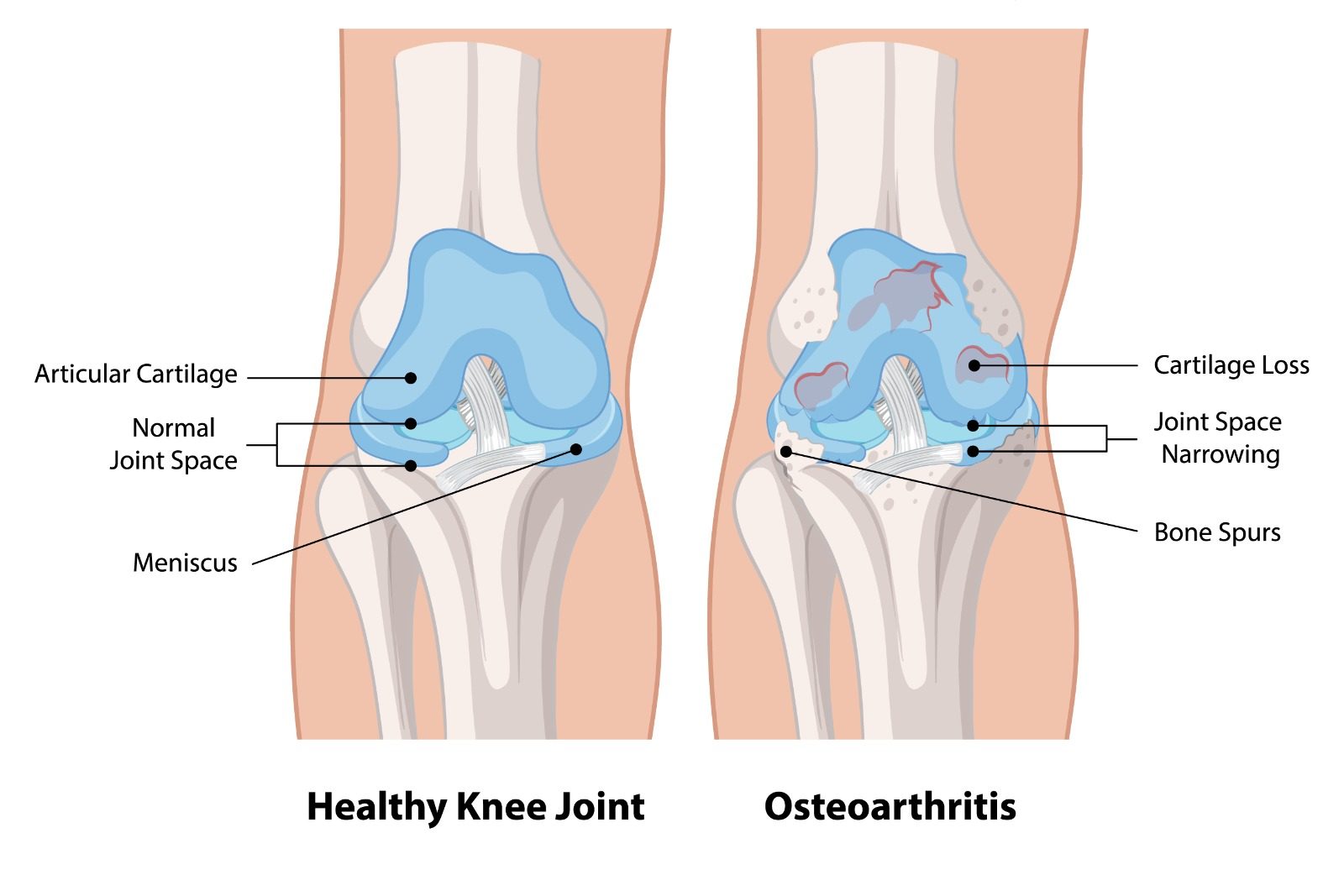
Articular cartilage is the smooth, glistening tissue covering the ends of bones within the knee joint, allowing frictionless movement. Cartilage injuries — also called chondral or osteochondral defects — occur when this cartilage is damaged, either through acute trauma or progressive wear. Unlike many other tissues, articular cartilage has virtually no inherent capacity to heal itself, as it lacks a direct blood supply. Untreated cartilage defects in young, active patients are a leading cause of premature knee osteoarthritis.
Causes & Risk Factors
- Direct impact or twisting injury — often associated with ACL tears or patellar dislocations
- Repetitive loading and microtrauma in high-impact sports
- Osteochondritis dissecans (OCD) — a condition in which a segment of bone and overlying cartilage loses its blood supply and separates from the surrounding tissue
- Knee malalignment (varus/valgus) concentrating load on one compartment
- Previous meniscal removal increasing joint contact stress
Signs & Symptoms
- Deep, aching joint pain aggravated by impact activities and weight-bearing
- Intermittent swelling of the knee joint
- Catching, locking, or a loose body sensation if a fragment has detached
- Joint line tenderness at the site of the defect
- Stiffness and pain after prolonged activity or sitting
Diagnosis
Standard X-rays may be normal in purely chondral defects. MRI with cartilage-specific sequences (T2 mapping, dGEMRIC) characterises defect size, depth, and bone involvement. Arthroscopy remains the gold standard for definitive assessment and classification (ICRS grading).
Treatment Options
- Bone marrow stimulation (microfracture): Creating small perforations in the bone to recruit stem cells — effective for smaller defects (< 2 cm²)
- Autologous Chondrocyte Implantation (ACI) / Matrix-induced ACI (MACI): Two-stage procedure harvesting and culturing the patient’s own cartilage cells for reimplantation — optimal for large defects in young patients
- Osteochondral Autograft Transfer (OATS/mosaicplasty): Transplanting cartilage plugs from a non-weight-bearing area to the defect — suitable for medium-sized defects
- Osteochondral allograft: Transplanting fresh cadaveric osteochondral tissue for large defects
- Addressing concomitant malalignment or ligament instability to protect cartilage repair
Patient FAQs – Knee Cartilage Injury (Osteochondral Defect)
Can knee cartilage grow back?
Articular cartilage cannot regenerate spontaneously. Biological repair procedures stimulate the formation of fibrocartilage (a less durable substitute) or allow implantation of cultured hyaline-like cartilage. These procedures reduce pain and improve function but do not fully replicate normal articular cartilage.
Is cartilage surgery effective?
Outcomes depend on defect size, location, patient age, and whether underlying causes are corrected. In appropriately selected young patients with isolated defects, MACI and osteochondral grafting provide excellent long-term outcomes with high rates of return to sport.
How long is recovery after cartilage surgery?
Cartilage procedures require extended protected rehabilitation. Non-weight-bearing typically lasts 6–8 weeks after MACI or osteochondral grafting, with return to sport at 12–18 months. Microfracture allows faster return (3–6 months) but for smaller defects.