Trigger Finger (Stenosing Tenosynovitis)
Overview
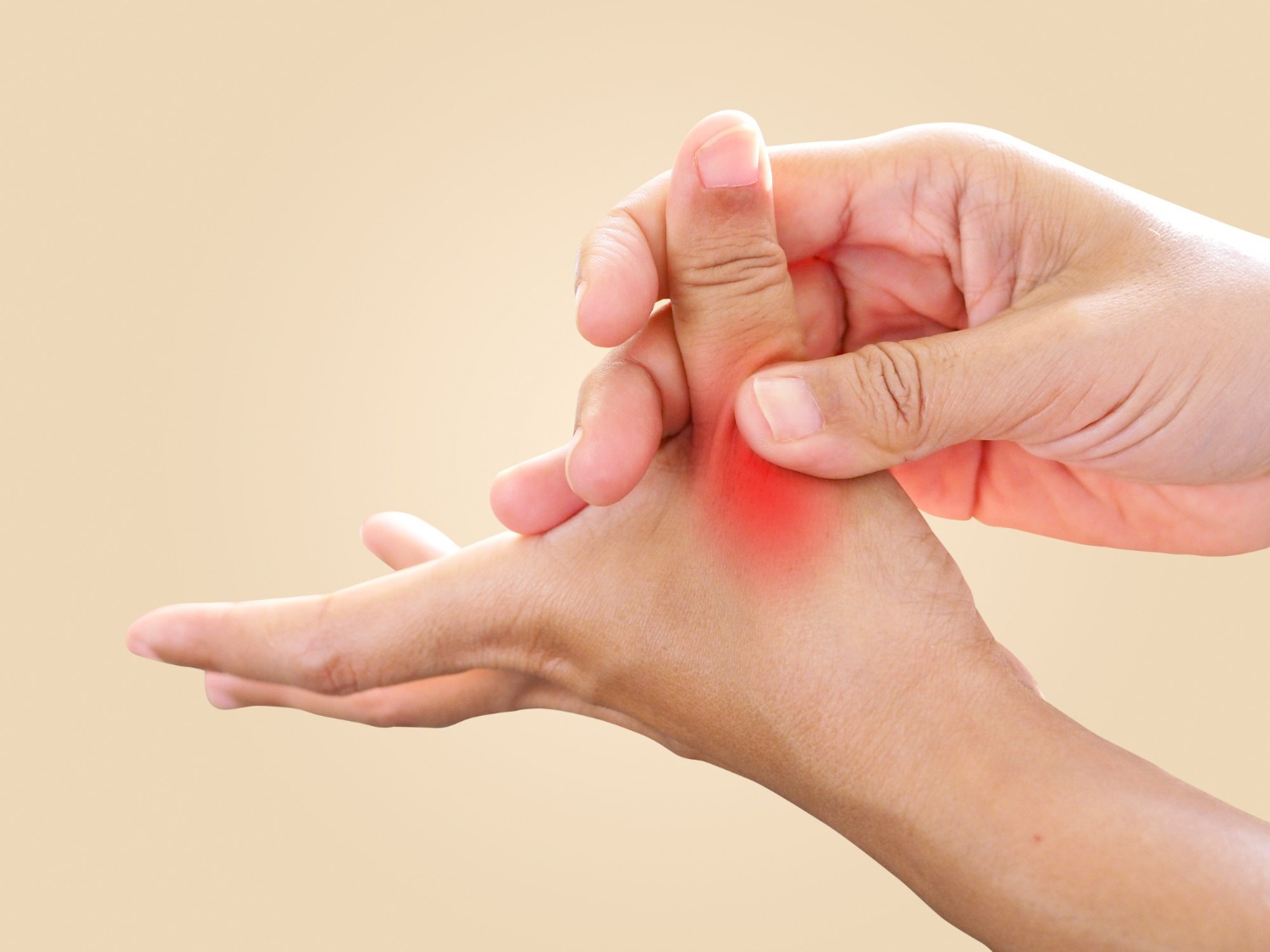
Trigger finger — formally termed stenosing flexor tenosynovitis — is a condition in which the flexor tendon of a finger (or thumb — trigger thumb) becomes intermittently caught at the entrance to the fibro-osseous flexor tendon sheath at the level of the A1 pulley, located at the base of the finger at the palmar metacarpal head. A nodular thickening develops on the tendon, and as the tendon attempts to glide through the narrowed A1 pulley, it catches or locks, producing the characteristic triggering, clicking, and in advanced cases a fixed flexion posture.
Causes & Risk Factors
- Idiopathic: Most common — no identifiable cause; cumulative mechanical stress on the A1 pulley and tendon
- Diabetes mellitus: Significantly increased risk (up to 10% of diabetics develop trigger finger); multiple digits commonly affected; poorer response to steroid injection
- Rheumatoid arthritis: Flexor tenosynovitis is a primary feature of RA; multiple trigger fingers are common
- Repetitive gripping activities: Occupational and recreational
- Most common in women aged 40–60; the middle and ring fingers and thumb are most frequently affected
Grading & Symptoms
Grade I (Pre-triggering) | Pain and tenderness at the A1 pulley. No catching. History of catching only. |
Grade II (Active Triggering) | Catching during active finger flexion or extension. Patient can self-correct the trigger. |
Grade III (Passive Triggering) | Locking in flexion. Requires passive correction with the other hand. |
Grade IV (Contracture) | Fixed flexion contracture — the finger is locked in flexion and cannot be passively extended. Requires urgent intervention. |
- Palpable and tender nodule at the A1 pulley (base of the finger, in the palm)
- A palpable click as the nodule passes through the pulley during finger movement
- Morning stiffness and locking — most severe on first use after prolonged rest
Treatment
Corticosteroid Injection (First-Line)
Injection of corticosteroid into the flexor tendon sheath at the A1 pulley level is the most effective non-surgical treatment and produces complete resolution in 60–90% of first-time injectors. Success rates are lower in diabetics, in longstanding cases, and when multiple digits are involved. A second injection is appropriate if partial improvement was achieved.
Surgical Release (A1 Pulley Division)
- Indicated when injection fails or symptoms recur after two injections, or for Grade IV contracture
- Performed under local anaesthesia (WALANT technique) as a day-case procedure
- A 1–2 cm incision at the base of the finger allows direct visualisation and complete longitudinal division of the A1 pulley, releasing the entrapped tendon
- The patient actively flexes and extends the finger on the table to confirm complete release before closure
- Recovery: Full finger movement from day 1; return to light work within 1–2 weeks; full grip-intensive activities within 4 weeks
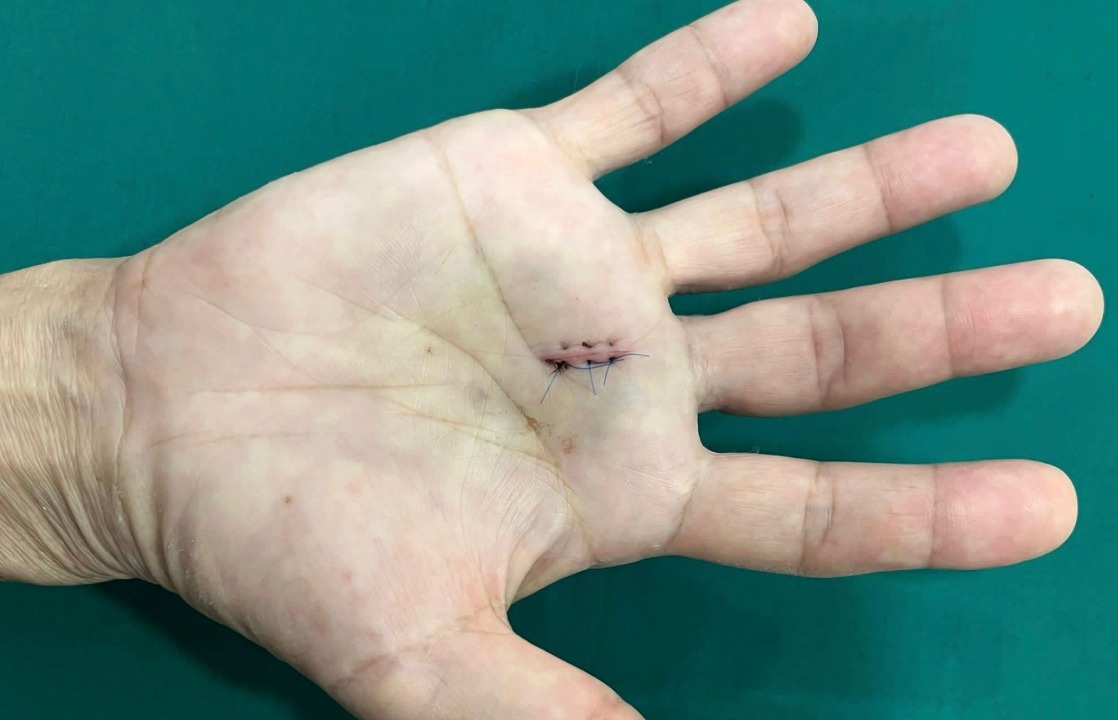
Percutaneous Release
- Indicated when injection fails or symptoms recur after two injections, or for Grade IV contracture
- Performed under local anaesthesia (WALANT technique) as a day-case procedure
- A 1–2 cm incision at the base of the finger allows direct visualisation and complete longitudinal division of the A1 pulley, releasing the entrapped tendon
- The patient actively flexes and extends the finger on the table to confirm complete release before closure
- Recovery: Full finger movement from day 1; return to light work within 1–2 weeks; full grip-intensive activities within 4 weeks
Patient FAQs –Trigger Finger (Stenosing Tenosynovitis)
My finger is locked — is this an emergency?
A finger locked in flexion (Grade IV) should be assessed promptly. While not a medical emergency, prolonged locking leads to flexion contracture of the proximal interphalangeal (PIP) joint that can become permanent. Please contact Dr. Senthilvelan’s clinic for an early appointment.
How many steroid injections can I have for trigger finger?
A maximum of two injections per digit is generally recommended. Beyond this, the risk of tendon weakening from repeated steroid exposure increases, and surgical release should be considered. If two injections fail to provide lasting relief, surgery is the definitive and highly effective next step.
My child has a thumb that locks — is this the same condition?
Paediatric trigger thumb is a different condition from adult trigger finger. It is caused by a congenital nodule (Notta’s node) on the flexor pollicis longus tendon. It rarely resolves spontaneously in children over 3 years and usually requires surgical release. Please arrange an early consultation.