Shoulder Arthritis
Treatment by Dr. Senthilvelan – Shoulder, Elbow & Wrist Specialist
Overview
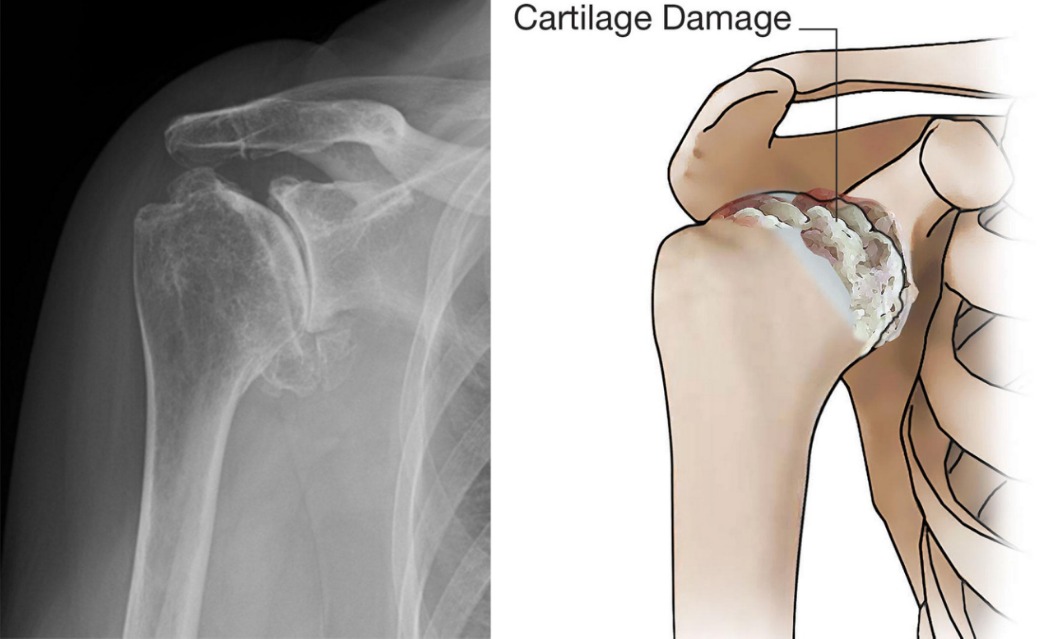
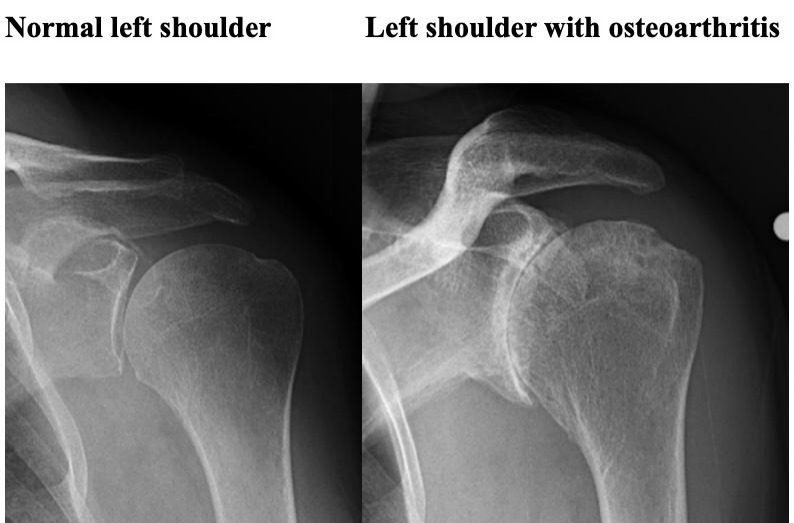
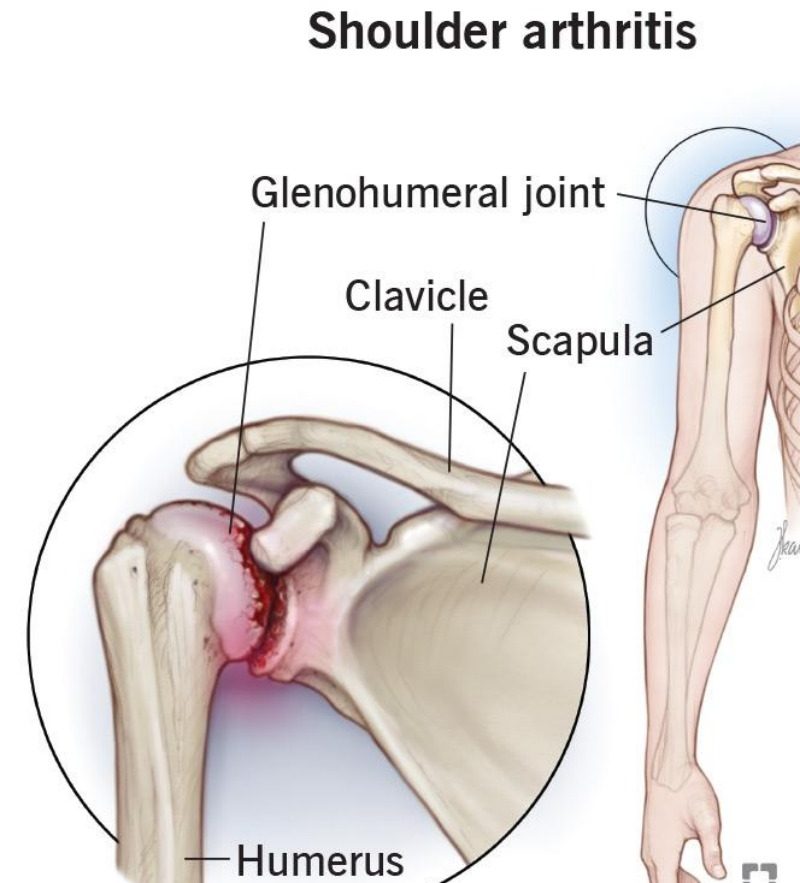
Shoulder Anatomy
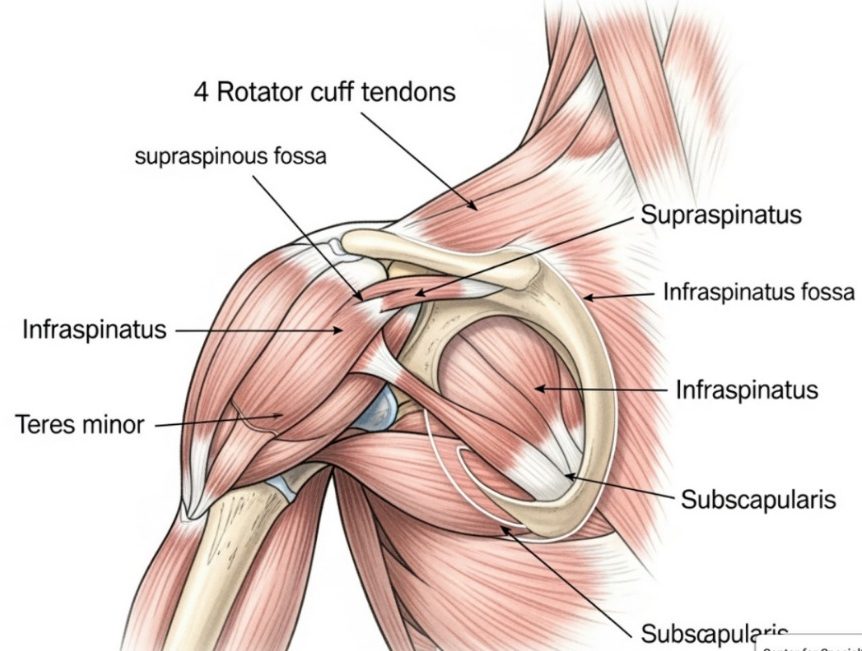
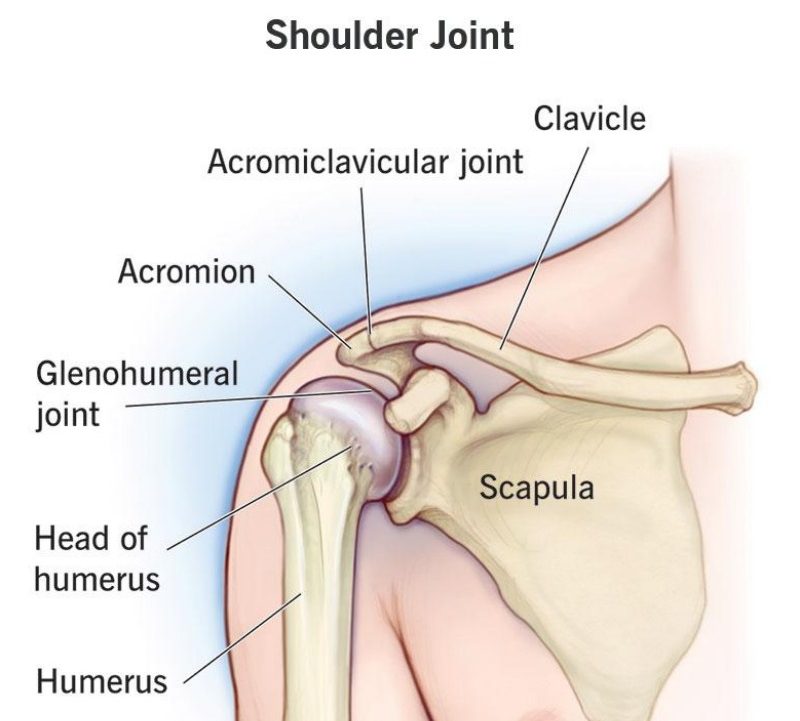
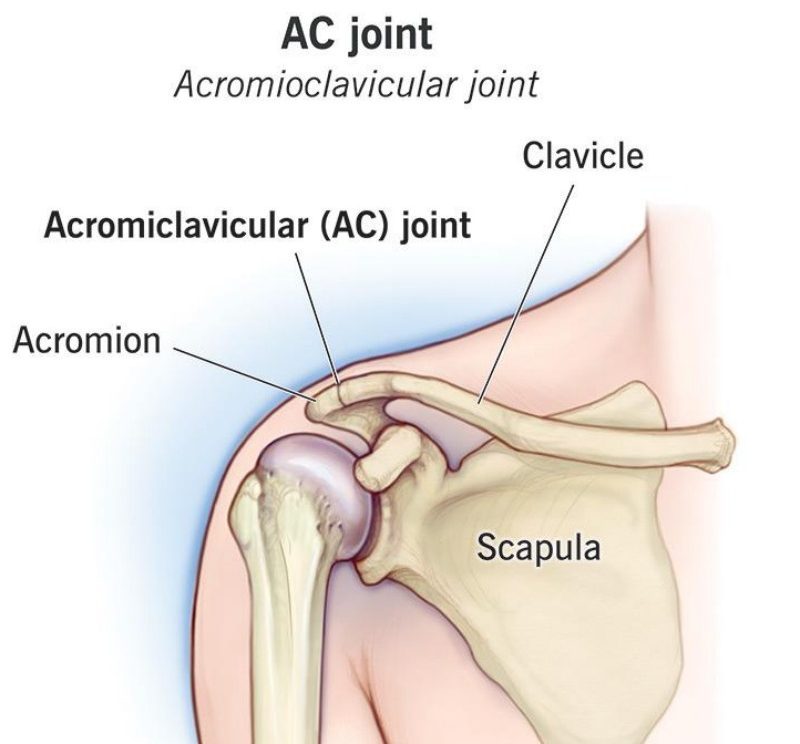
Types of Shoulder Arthritis
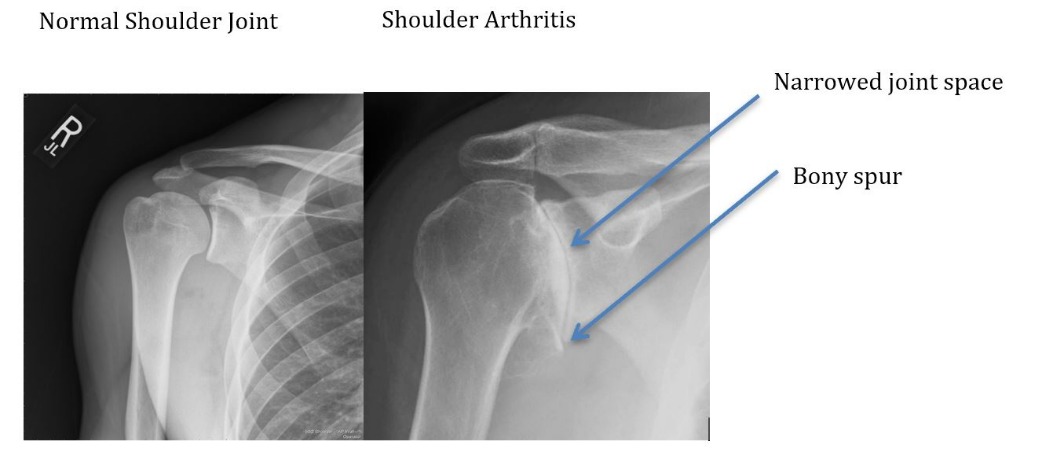
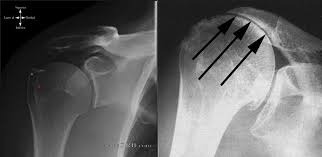
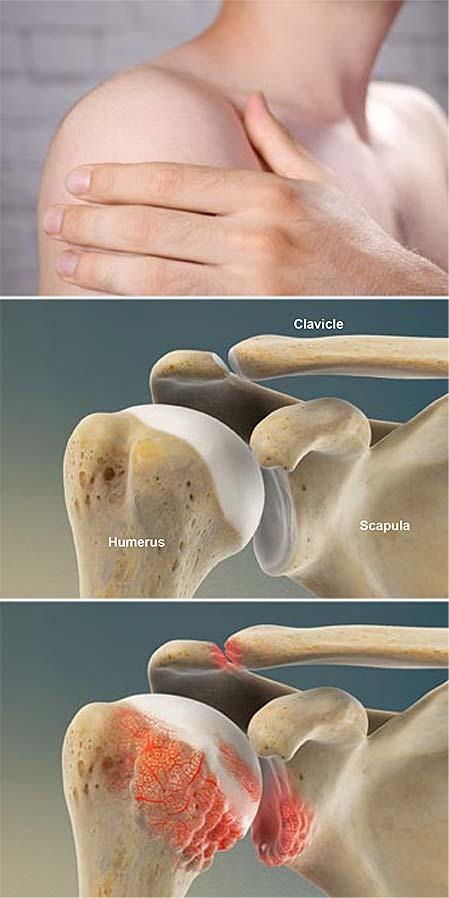
- Osteoarthritis Also called “wear-and-tear” arthritis Caused by gradual cartilage degeneration More common after age 50 Often affects the AC joint, but glenohumeral arthritis causes more symptoms
- Rheumatoid Arthritis Autoimmune condition Body’s immune system attacks joint lining Usually affects both shoulders symmetrically Causes pain, swelling, and stiffness
- Post-Traumatic Arthritis Develops after shoulder injuries Common after fractures or dislocations Can affect either shoulder joint
-
Rotator Cuff Tear Arthropathy Occurs after long-standing large rotator cuff tears The humeral head moves upward due to lack of tendon support Leads to severe arthritis and weakness
- Avascular Necrosis (AVN) Caused by loss of blood supply to the humeral head Bone gradually collapses Leads to arthritis
-
Common causes of AVN: High-dose steroid use Excessive alcohol consumption Sickle cell disease Trauma Unknown causes (idiopathic)
Causes and Risk Factors
- Age-related degeneration
- Previous shoulder injuries
- Autoimmune diseases
- Rotator cuff tears
- Steroid use
- Alcohol abuse
- Metabolic conditions
Symptoms of Shoulder Arthritis
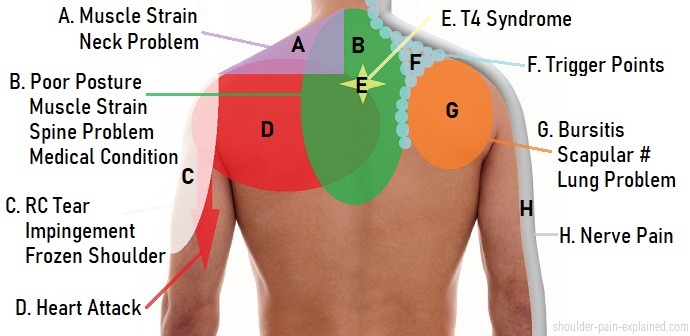
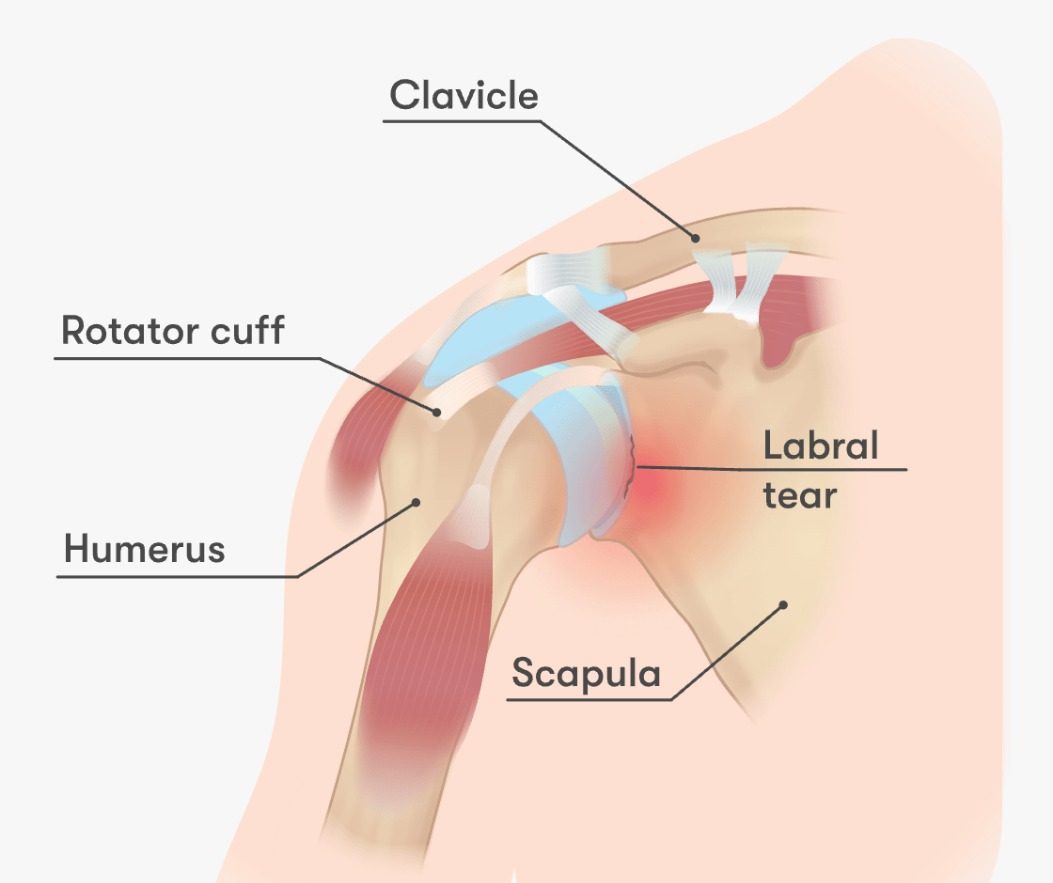
Evaluation by Dr. Senthilvelan
- Muscle strength testing
- Range of motion evaluation
- Joint tenderness
- Crepitus during movement Assessment of surrounding tendons and ligaments
- Examination of other joints (if rheumatoid arthritis suspected)
Imaging Investigations
- X-rays
- Joint space narrowing
- Bone spurs
- Joint deformity
- CT Scan Used for surgical planning
- Diagnostic Injection
- Local anesthetic injected into the joint
- If pain improves, arthritis is confirmed as the source
Non-Surgical Treatment
- Initial treatment is usually conservative.
- Treatment Options
- Activity modification
- Physiotherapy to improve mobility and strength
- Anti-inflammatory medications
- Corticosteroid injections
- Heat or ice therapy
- In rheumatoid arthritis, disease-modifying medications may be prescribed in coordination with a rheumatologist.
Surgical Treatment
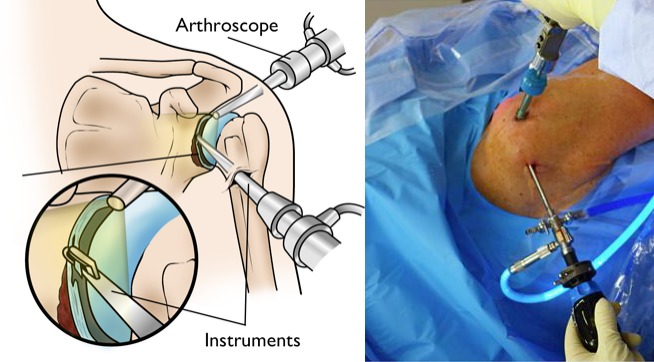
1) Arthroscopic Debridement (Early Arthritis)
Minimally invasive keyhole surgery
Removal of loose cartilage
Cleaning inflamed tissue
Smoothing bone spurs
Best for: Early or mild arthritis Younger patients
Note: Relief may be temporary in advanced arthritis.
2) Shoulder Replacement Surgery (Advanced Arthritis)
In shoulder replacement, the damaged joint surfaces are replaced with artificial components.
a) Hemiarthroplasty
Only humeral head replaced Used in selected cases
b) Total Shoulder Replacement
Both ball and socket replaced Best for patients with intact rotator cuff
c) Reverse Shoulder Replacement
Ball and socket positions reversed Relies on deltoid muscle instead of rotator cuff
Ideal for:
Rotator cuff tear arthropathy
Elderly patients with severe arthritis
Recovery After Surgery
Possible Surgical Risks
- Infection
- Bleeding
- Blood clots
- Nerve or vessel injury
- Implant-related complications